Table of Contents
At a Glance
|
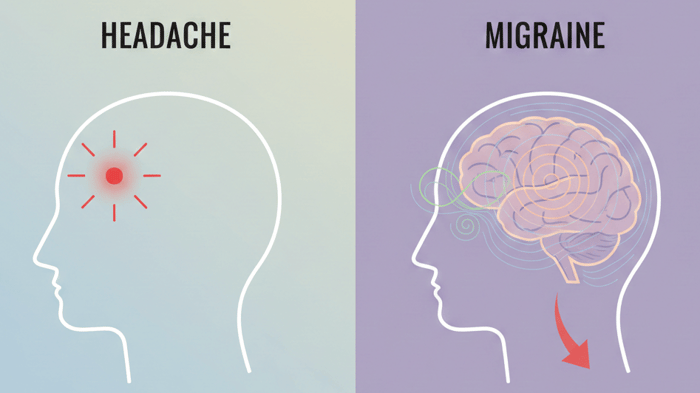
Facial pressure, pain around the eyes, and a sense of congestion are often assumed to point to a sinus problem. However, many of these episodes are actually migraine, which can produce similar sensations even when the sinuses are clear.
Understanding the key differences between sinus headache vs migraine therefore involves more than identifying where pain is felt. The timing of symptoms, associated features, and how they change over time often provide clearer clues than location alone.
What Is a Sinus Headache?
The sinuses are air-filled spaces located behind the forehead, cheeks, and eyes that help humidify and filter the air you breathe. When these cavities become inflamed or blocked during an acute sinus infection, pressure can build, leading to facial pain and tenderness. A sinus headache refers to head pain that arises from this inflammation within the sinus cavities (Rosenfeld et al., 2015).
Sinus headache pain is typically felt in the forehead, around or behind the eyes, across the cheeks, or in the upper teeth. It often worsens when bending forward or with sudden head movement, reflecting pressure changes within the sinus cavities. Unlike migraine, sinus headaches are usually accompanied by clear signs of infection, such as thick or discolored nasal discharge, nasal congestion, reduced sense of smell, or fever.
Sinus headaches tend to develop alongside other symptoms of sinusitis rather than in isolation. Facial tenderness is common, particularly when pressure is applied to the cheeks or forehead. This discomfort typically remains consistent throughout the infection and improves gradually as inflammation settles.

Although these symptoms are well recognized, true sinus-related headaches are relatively uncommon compared with migraine (Schreiber et al., 2004). Many recurrent sinus headaches are later found to be migraine, especially when signs of infection are absent. Therefore, the presence of infection-related symptoms is a key factor in distinguishing sinus headache from migraine.
Not all head pain around the face reflects sinus inflammation. Tension-type headaches typically produce a steady, band-like pressure without signs of infection, while cluster headaches cause brief but extremely intense one-sided attacks often centered around the eye and accompanied by tearing or nasal symptoms. Although pain may occur in similar areas, these conditions differ in timing, associated features, and underlying mechanisms. Recognizing these broader headache categories helps clarify why recurrent facial pain is not always sinus-related and may instead reflect migraine rather than another type of headache.
What Is a Migraine?
Migraine is a neurological condition involving more than head pain alone. It reflects a change in how the brain processes sensory information, regulates energy use, and modulates pain signals. Head pain is only one part of this state and may not always be the most prominent feature.
Migraine pain is often described as throbbing or pulsating and usually affects one side of the head, though it can involve both sides or even shift between them. Discomfort often worsens with routine activities such as walking, climbing stairs, or bending, and migraine is frequently accompanied by sensitivity to light, sound, or smell. Nausea, fatigue, difficulty concentrating, and dizziness are also common symptoms.
Some people experience aura, which involves temporary neurological symptoms such as visual disturbances, tingling sensations, or speech difficulty. Aura does not occur in all migraine and may appear without significant head pain, sometimes referred to as aura migraine without headache. In some people, aura episodes can also occur repeatedly over a short period.
Unlike sinus headache, which usually develops alongside an infection in the sinuses, migraine tends to unfold as a broader episode affecting multiple body systems at once. Symptoms often build gradually, fluctuate in intensity, and may continue even after head pain improves. Many people notice early warning signs such as yawning, food cravings, neck discomfort, or changes in mood before pain begins, followed by a recovery phase marked by tiredness or mental slowing.
Migraine usually recurs over time in recognizable patterns. Triggers such as sleep disruption, hormonal changes, sensory overload, dehydration, or missed meals can lower the brain’s tolerance to stimulation by reducing its ability to regulate incoming sensory signals, making it more sensitive to light, sound, movement, or internal signals and increasing the likelihood of migraine occurrence. Because migraine reflects altered brain responsiveness rather than local inflammation, symptoms can occur even when tests appear normal.
To explore migraine in more detail, including triggers, causes, and practical management strategies, see: What Causes Migraines, Understanding Migraine Triggers, Hormones and Migraines: What You Need to Know, Can Migraines Cause Neck Pain?, and How to Get Rid of a Migraine at Home.
Why Migraine Can Feel Like a Sinus Headache
Migraine can produce facial pressure, discomfort around the eyes, and nasal symptoms that closely resemble a sinus problem, even when no infection is present. This overlap reflects shared nerve pathways in the face and sinus region, even though the underlying biological processes are distinct.
The trigeminal nerve supplies sensation to the face, forehead, eyes, and sinuses. During migraine episodes, activation of trigeminal pain pathways can also generate discomfort in these regions (Goadsby et al., 2017). Pain felt behind the eyes, across the forehead, or around the cheeks may therefore reflect altered nerve signaling rather than indicating inflammation within the sinus cavities.
Migraine can also involve changes in the body’s automatic nerve responses, including nasal congestion or watery discharge. These symptoms arise from nerve activation linked to migraine pain pathways, not from sinus infection or blockage. Because these sensations resemble common sinus symptoms, migraine is often misinterpreted as sinus-related.
The distinction lies in what drives the symptoms. Sinus headache is linked to inflammation within the sinus cavities during acute infection. Migraine reflects altered sensory processing and pain modulation within the nervous system. Although discomfort may occur in similar areas, the mechanisms involved are different.
Shared nerve anatomy helps explain why facial pain alone cannot reliably distinguish sinus headache from migraine.

How Symptom Patterns Differ Over Time
Another useful way to distinguish sinus headache from migraine is to consider how their symptoms behave over time.
A true sinus headache typically develops alongside an acute sinus infection. Facial pressure, nasal discharge, and tenderness tend to appear together and remain relatively consistent during illness. As the infection clears, symptoms typically settle gradually.
Sinus headaches usually improve as nasal inflammation settles, whereas migraine symptoms often persist despite sinus treatments. Once resolved, symptoms usually clear without ongoing sensitivity unless another infection develops.
Migraine follows a different trajectory from sinus headache, with symptoms that tend to build gradually rather than appearing all at once. Facial pressure or eye discomfort can be accompanied by fatigue, light sensitivity, nausea, or cognitive slowing. Symptoms can fluctuate in intensity over several hours to several days, shifting in prominence as the episode progresses. Head pain may ease at certain stages, even while other features remain noticeable.
Recurrence is also an important distinction. Sinus headache is usually linked to a discrete illness episode, whereas migraine tends to recur in recognizable patterns, sometimes with similar accompanying features across episodes. Sensitivity or tiredness may also persist after pain subsides.
The way symptoms develop, fluctuate, and recur over time often distinguishes the two conditions more clearly than pain location alone.
Sinus Headache vs Migraine: Key Differences
Sinus headache and migraine can both cause facial pain and pressure, yet they arise through different biological processes that behave differently over time. Paying attention to how symptoms develop, what accompanies them, and how they settle can often provide clearer insights than the location of pain alone.
The table below highlights the most consistent differences between sinus headache and migraine. These patterns reflect common trends rather than strict diagnostic rules and help explain why the two conditions are frequently confused and often respond differently to treatment.
Table of differences: migraine vs sinus headache
Feature | Sinus Headache | Migraine |
Underlying cause | Local inflammation related to acute sinus infection | Altered brain responsiveness involving sensory processing and pain modulation |
Typical trigger | Sinus infection or severe nasal inflammation | Sleep disruption, sensory load, hormonal shifts, or metabolic strain |
Pain location | Face, forehead, or behind the eyes, often with facial tenderness | Often one-sided but can involve forehead, eyes, jaw, or whole head |
Nasal symptoms | Thick or discolored nasal discharge is common | Nasal congestion may occur without signs of infection |
Fever or infection signs | Often present | Absent |
Effect of bending forward | Pain often worsens | Usually no consistent effect |
Sensitivity to light or sound | Usually absent | Common and often prominent |
Associated symptoms | Primarily facial pressure and pain | Nausea, fatigue, dizziness, cognitive slowing, or sensory sensitivity |
Symptom pattern over time | Stable during illness and improves as infection clears | Symptoms often build, fluctuate, and recur in similar patterns |
Duration | Days to weeks, resolving with infection | Hours to days, with possible lingering sensitivity |
Between episodes | Symptom-free once infection resolves | Sensitivity or fatigue may persist even without head pain |
One particularly helpful clue is sensitivity to light or sound, which strongly favors migraine rather than sinus headache. These differences help clarify why migraine can be mistaken for a sinus headache when facial pressure or nasal symptoms are prominent. In most cases, sinus headache is linked to active infection, whereas migraine reflects a recurring neurological pattern that can occur even without evidence of sinus infection.
Why Sinus Headache and Migraine Are Often Confused
Sinus headaches and migraine feel similar because they produce pain in similar areas around the forehead, eyes, and cheeks. When facial pressure is present, it is easy to assume the sinuses are responsible, even if the cause lies elsewhere. Understanding the difference between migraine and sinus headache therefore depends on looking beyond pain location alone.
Common reasons the two are mixed up:
Location of pain overlaps: both can affect the forehead, around the eyes, and the upper face
Facial pressure occurs in migraine: pressure does not always indicate sinus inflammation
Nasal symptoms can appear in migraine: congestion or watery discharge may occur without infection
Colds often trigger migraine episodes: the timing makes symptoms seem sinus-related
Seasonal allergies can trigger migraine: congestion during allergy flares can be mistaken for sinus inflammation
Bending forward can worsen either: increased pressure sensation is not unique to sinus disease
Migraine may not always be throbbing: milder attacks can feel like steady pressure
Migraine can also cause discomfort in the teeth or jaw through shared nerve pathways, sometimes mistaken for dental or sinus pain. Learn more about migraine tooth pain and whether wisdom teeth can cause migraine headaches.
Brain Ritual® and Migraine Support
Facial pressure resembling sinus discomfort is often part of migraine, a condition associated with changes in brain energy use and increased oxidative stress within sensory pathways.
The Brain Ritual® formula includes ketone bodies such as D-beta-hydroxybutyrate, which serve as an alternative fuel source for brain cells during periods of higher demand, along with nutrients involved in mitochondrial energy production and antioxidant balance, including riboflavin, magnesium, and CoQ10.
Ingredients commonly discussed in relation to normal immune and mucosal function, such as vitamin C, zinc, selenium, vitamin A, and vitamin D, are also present in the formulation. Their inclusion does not target sinus disease specifically but reflects the broader nutritional composition of Brain Ritual®.
Learn more about and purchase Brain Ritual® medical food here.
Disclaimer: Brain Ritual® is a medical food for the dietary management of migraine and is not intended to diagnose, treat, cure, or prevent any disease. This content is for informational and educational purposes only and is not intended as medical advice.
Final Thoughts
Understanding whether symptoms reflect migraine or sinus headache often comes down to the overall pattern of symptoms rather than where the pain is felt. Both can cause facial pressure and discomfort around the eyes, but sinus headache is typically linked to infection, whereas migraine is a recurring neurological process and can occur even when the sinuses are clear.
Looking at accompanying symptoms and how episodes develop over time can help clarify what is actually happening. Recognizing that there is a migraine pattern behind facial pain helps explain why sinus treatments often have little effect and can guide more appropriate care.