Table of Contents
- What Makes Migraine Different from Other Headaches?
- Why Migraine Is Often Mislabeled as Just a Headache
- How Migraine Differs from Other Common Headaches
- Why Treating Migraine as a Headache Often Falls Short
- How to Think About Migraine vs Headache Going Forward
- Supporting Migraine Stability with a Structured Nutritional Approach
- Frequently Asked Questions
- Final Thoughts
At a Glance
|
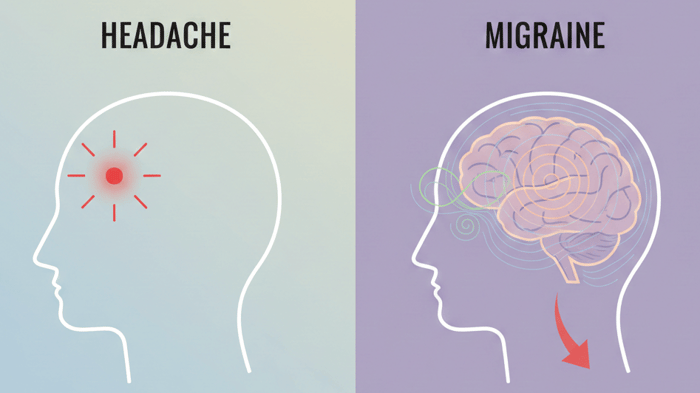
Headache is often used as a catch-all term for head pain. This broad label can hide important differences in how symptoms arise and behave. An understanding of the difference between migraine vs headache goes beyond the severity or location of pain and instead reflects underlying biological processes. For example, similar sensations such as pressure, throbbing, and pain around the eyes can emerge through very different biological pathways.
Migraine is not defined by pain alone. Instead, it reflects a broader state of altered brain responsiveness that can affect sensory processing, energy regulation, and how the nervous system responds to internal and external stress. Common headache types, such as tension, sinus, and cluster headaches, involve head pain but are shaped by different mechanisms and tend to follow more specific patterns.
Recognizing these differences helps explain symptom overlap, migraine’s unpredictable nature, why people often ask are headaches and migraines the same, and why approaches aimed only at relieving local pain or inflammation do not always bring relief.
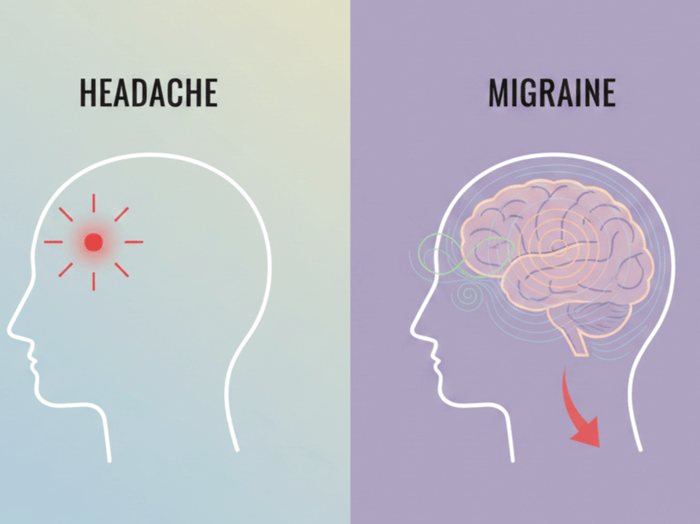 Image Caption
Image CaptionWhat Makes Migraine Different from Other Headaches?
Migraine differs from other headache types because it reflects altered brain responsiveness to internal and external signals (Charles et al., 2018). Though pain is often the most visible feature, it is only one expression of a wider neurological state that can influence sensory processing, energy regulation, and autonomic function.
Migraine involves multiple interacting brain systems, rather than a single structure or tissue (Ferrari et al., 2021). This helps explain why symptoms often extend beyond head pain and may occur even when pain is mild or absent.
Migraine as a State of Altered Brain Responsiveness
During migraine, the brain tends to operate in a more sensitive and reactive state. Sensory inputs normally filtered or tolerated can feel amplified, while physiological demands that are usually manageable may become taxing.
Altered brain responsiveness is not constant and can fluctuate over time, influenced by factors such as hormonal changes, sleep quality, metabolic demand, stress load, and cumulative sensory input. This means migraine symptoms often vary from day to day and do not always follow a predictable pattern.
Pain Is Only One Expression of Migraine
Migraine activity can occur independently of head pain. Some people experience migraine episodes dominated by visual changes, nausea, dizziness, fatigue, or sensory sensitivity, with little or no head pain.
This helps explain why migraine can sometimes be mistaken for other conditions or dismissed when pain does not fit a familiar pattern. It also explains why treating pain alone does not always address the underlying process driving migraine symptoms.
Sensory Amplification
One of the most consistent features of migraine is heightened sensory sensitivity. Light, sound, smell, movement, and touch may feel overwhelming during migraine.
This sensory amplification arises from how the brain processes incoming signals, rather than from irritation of the eyes, ears, or other sensory organs themselves. It also helps explain why everyday environments can feel intolerable during migraine and why withdrawing to quiet, dark spaces is a common way people try to reduce sensory input.
Altered Energy Metabolism
Migraine is closely linked to how the brain manages energy (Gross et al., 2019). During migraine, the brain tends to operate closer to its metabolic limits, making it more sensitive to changes in energy demand. Physical exertion, sustained cognitive effort, missed meals, and disrupted sleep can all place additional strain on systems that are already working less efficiently.
This energy strain can contribute to fatigue, brain fog, slowed thinking, and delayed recovery after migraine episodes. It also helps explain migraine’s sensitivity to metabolic stress and the tendency for symptoms to worsen with exertion rather than improve.
When energy production becomes less efficient, the brain is more vulnerable to oxidative stress, reflecting a mismatch between metabolic demand and the brain’s ability to neutralize reactive byproducts of energy metabolism. In migraine, this oxidative burden is thought to significantly lower tolerance to sensory input, exertion, and stress, reinforcing a broader state of heightened sensitivity rather than acting as a single, isolated trigger (Borkum et al., 2016).
Because migraine appears sensitive to how energy is supplied and used, there has been growing interest in alternative fuel sources that place different energy-processing demands on the brain. Ketone bodies, for example, provide an efficient energy substrate that generates fewer reactive byproducts during metabolism compared with glucose. This perspective helps illustrate why migraine is often described as an energy-vulnerable brain state rather than a condition driven by pain alone.
Neurotransmitter and Brainstem Involvement
Migraine involves changes in chemical signaling between nerve cells, affecting systems responsible for pain perception, sensory filtering, and arousal. These changes influence how strongly sensory and pain-related signals are amplified, and how easily the brain shifts between states of activation and recovery.
The brainstem (which helps regulate arousal, pain modulation, and autonomic function) and the trigeminovascular system (the main network carrying sensory and pain signals from the face and head) play a coordinating role in this process, linking sensory input, autonomic responses, and pain pathways. This integration helps explain why migraine affects multiple body systems at once, rather than producing isolated symptoms more typical of common headache types.
Autonomic and Regulatory Symptoms
Many migraine symptoms reflect involvement of the autonomic nervous system. Nausea, vomiting, temperature sensitivity, altered sweating, and gastrointestinal discomfort are all common features of migraine that are not typically explained by head pain alone.
These autonomic symptoms reinforce the idea that migraine is a whole-brain condition that affects regulation and not just sensory perception. They also help distinguish migraine from headache types driven primarily by local tissue irritation or inflammation.
Migraine With or Without Head Pain
Migraine reflects a broader neurological state that can remain active between attacks or even when significant head pain is absent. This helps explain why some people experience ongoing sensitivity, fatigue, or cognitive symptoms even when they are not experiencing what feels like a migraine headache.
It also explains why triggers do not usually cause migraine in isolation. Instead, they tend to expose an underlying vulnerability in a brain that is already operating closer to its tolerance threshold.
Why Migraine Is Often Mislabeled as Just a Headache
Migraine is frequently reduced to the idea of a headache because pain is the most visible and familiar symptom. In common use and even in some clinical settings, head pain becomes shorthand for migraine, while the broader neurological features are overlooked.
This simplified way of thinking creates confusion, particularly because migraine does not always present as a dramatic or disabling headache. Pain intensity can vary widely, and for some people it may be mild, intermittent, or absent altogether. When migraine does not fit the expected image of severe head pain it can sometimes be dismissed or misclassified.
Another source of confusion lies in the episodic nature of migraine. Symptoms may build gradually, fluctuate, or linger after head pain has resolved. Fatigue, sensory sensitivity, cognitive slowing, and nausea can precede a migraine episode or persist long after pain has eased, making it difficult to recognize where an attack begins or ends.
Migraine can also present in less typical ways, making it harder to recognize. Many people with migraine also experience aura, which refers to temporary neurological symptoms such as visual changes, tingling, or speech disturbance. However, migraine does not require aura, and many people never experience these symptoms at all. Others experience what is known as silent migraine, where neurological or autonomic symptoms occur without significant head pain. In these cases, migraine activity may be present but go unrecognized.
Together, these factors help explain why migraine is often thought of as just a headache. When attention is focused mainly on pain the broader neurological state behind symptoms may be overlooked. This misunderstanding can lead to poor comparisons, delayed recognition, and approaches that focus on surface symptoms rather than the broader migraine process.
How Migraine Differs from Other Common Headaches
Migraine is often confused with other headache types because head pain can arise through multiple biological pathways. In practice, migraine involves a distinctive neurological pattern, with other headache types more closely linked to peripheral pain signaling, inflammation, or autonomic activation. By understanding these differences, it becomes clearer why symptoms can feel similar at first, yet behave very differently over time.
Key Differences Between Migraine and Other Headaches
Although migraine and other headaches often overlap in how they feel, they differ in several consistent ways. These differences help explain why migraine often behaves as a recurring pattern rather than as a single pain episode.
Pain Characteristics
Headache: Pain is often dull, tight, or pressure-like, typically mild to moderate in intensity, and commonly felt on both sides of the head.
Migraine: Pain more often feels throbbing, pulsating, or stabbing, is moderate to severe in nature, and tends to affect one side of the head, though it can switch sides.
Response to Movement
Headache: Symptoms often remain stable or may improve with gentle movement or changes in posture.
Migraine: Symptoms often worsen with physical activity such as walking, bending, or light exertion, and tend to ease with rest.
Associated Symptoms
Headache: Usually limited to head pain, with few additional sensory or systemic symptoms.
Migraine: Commonly involves symptoms beyond pain, including nausea or vomiting, sensitivity to light, sound, or smell, visual disturbances such as aura, fatigue, brain fog, neck discomfort, and changes in mood or energy before pain begins. Migraine activity can also occur without significant head pain, sometimes referred to as silent migraine.
Timing and Symptom Patterns
Headache: Typically follows a straightforward course, with pain that develops and resolves without a distinct sequence of phases.
Migraine: Often unfolds as a sequence, beginning with early changes sometimes referred to as the prodrome, such as fatigue, yawning, cravings, or irritability, followed in some people by aura, a phase of head pain or other symptoms, and a lingering recovery period often called the postdrome. This multi-phase pattern is not typical of most non-migraine headaches.
Together, these key differences help explain why migraine is often harder to recognize and manage when it is treated as just another headache. Migraine tends to behave as a broader neurological state that unfolds over time, rather than a single episode of head pain.
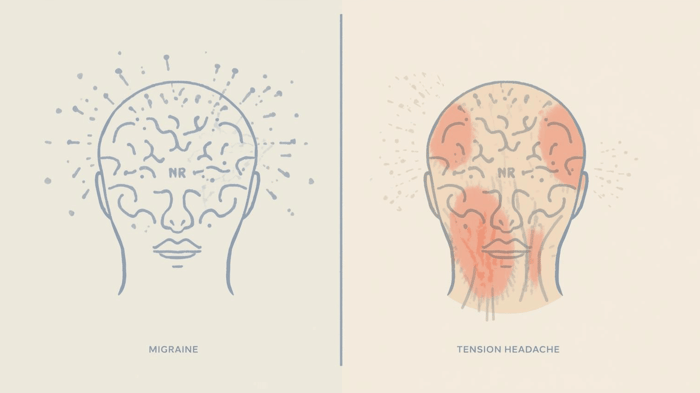
Migraine vs Tension Headache
Migraine and tension-type headaches are often grouped together, even though they arise through different biological pathways.
Tension headache is most commonly linked to sustained muscle tension, postural strain, and peripheral pain signaling from the neck, shoulders, or scalp. The pain is often described as dull, pressure-like, or band-shaped, as though a tight pressure is wrapping around the head, and tends to stay relatively stable rather than fluctuating. Sensitivity to light or sound is usually minimal, so everyday activities often remain manageable.
Migraine reflects a state of heightened neurological sensitivity. The pain may be throbbing or one-sided, but it is more often accompanied by sensitivity to light or sound, nausea, fatigue, cognitive slowing, or, in some cases, neurological symptoms such as visual aura. These features point to altered sensory processing rather than local muscle tension alone.
Another difference between migraine and tension headache lies in how symptoms change over time. Migraine tends to fluctuate over hours or days, and may be influenced by factors such as sleep disruption, hormonal shifts, energy demand, or cumulative stress. By comparison, tension headaches are more closely linked to ongoing physical or emotional strain and often improve with rest or postural change. Although neck or shoulder tightness can occur during migraine, it is usually part of a broader pattern of brain sensitivity rather than the primary driver of pain.
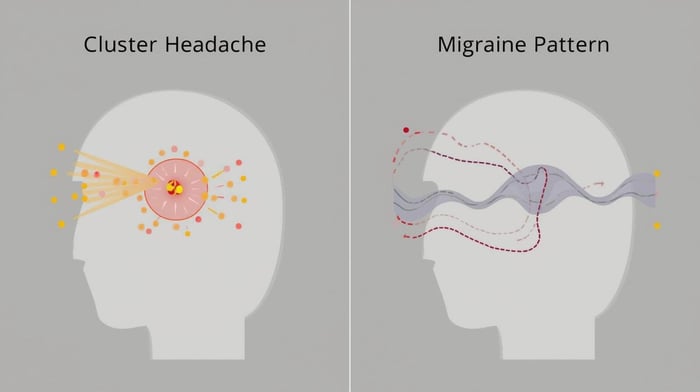
Migraine vs Cluster Headache
Migraine and cluster headaches are both neurological in origin, but they follow very different patterns.
Cluster headache is marked by short-lasting but extremely intense attacks that occur in predictable cycles, often referred to as clusters. Pain is usually focused around one eye or temple, and is commonly accompanied by autonomic symptoms such as tearing of the affected eye, nasal congestion, facial flushing, or eyelid drooping. During attacks, restlessness is common, with people often feeling unable to sit or lie still.
Migraine typically unfolds over a longer, less rigid timeframe than cluster headaches. Attacks may last many hours or days and are often preceded by subtle shifts in energy, mood, or sensory tolerance. Rather than producing sudden, intense autonomic symptoms, migraine tends to reflect a broader change in how the brain responds to sensory input, physical exertion, and internal stress.
Although both conditions involve trigeminal nerve pathways, the timing and structure of attacks differ markedly. Cluster headache tends to follow a tightly timed, repetitive pattern, often linked to specific times of the day or year. Migraine behaves more variably, with symptoms shaped by internal factors such as sleep disruption, hormonal shifts, metabolic demand, and cumulative stress.
These differences help explain why cluster headaches are often sharply episodic and time-bound, while migraine tends to behave as a more fluctuating, whole-brain condition.
Migraine vs Sinus Headache
Migraine and sinus headaches are often confused with each other because they produce similar sensations around the face and eyes.
True sinus-related headache is usually linked to acute sinus infection and is accompanied by clear signs of inflammation, such as fever, thick nasal discharge, and facial tenderness that worsens with head movement. These headaches are relatively uncommon and tend to resolve as the underlying infection clears.
Migraine can also cause facial pressure, nasal congestion, and discomfort around the eyes. This symptom overlap occurs because migraine and sinus structures share nerve pathways, particularly through the trigeminal system, which carries sensory signals from the face and sinuses to the brain. When pain is felt behind the eyes or across the forehead, migraine can be mistaken for a sinus problem, even in the absence of infection.
Unlike sinus headache, migraine is usually accompanied by sensitivity to light or sound, nausea, fatigue, or a worsening of symptoms during routine activity. Symptoms often recur in a similar pattern, rather than appearing only during a sinus-related illness.
These differences help explain why many people initially diagnosed with recurrent sinus headaches are later found to be experiencing migraine. The distinction matters because migraine involves altered sensory processing and brain responsiveness, whereas a true sinus headache is driven by localized inflammation related to infection.
Why These Headache Distinctions Matter
Although all three headache types involve head pain, they arise through different biological pathways. Migraine reflects a broader neurological state, whereas tension and sinus headaches are more closely tied to peripheral or inflammatory processes, and cluster headache represents a highly specific autonomic pattern. Recognizing these differences helps explain why migraines often behave unpredictably and may fail to respond to approaches aimed solely at relieving muscle tension or local inflammation.
Why Treating Migraine as a Headache Often Falls Short
Understanding the difference between migraine and other types of headache is important because the way symptoms are interpreted shapes how they are managed. When migraine is treated as a headache, attention tends to focus narrowly on pain relief, while broader underlying symptoms are left unaddressed.
This mismatch helps explain why migraine can feel stubborn and unpredictable. Approaches designed for tension, sinus, or other peripheral headaches often focus on local pain relief and may temporarily reduce discomfort, but they do not account for the underlying sensitivity of the migraine brain. As a result, symptoms may persist, quickly return, or shift in form instead of fully settling.
Migraine is sensitive to cumulative load, with energy demand, sleep disruption, sensory input, hormonal changes, and stress often interacting to gradually reduce tolerance. When viewed through a headache-only lens, this load-stacking effect may be missed, making it frustrating to identify what is really driving your migraine.
Energy and metabolic strain play an important role in migraine. Unlike some other headache types, migraine symptoms may worsen when the brain is under sustained demand, reflecting difficulty meeting ongoing energy needs. When this pattern is overlooked, attempts to manage symptoms can unintentionally increase strain rather than reduce it.
When migraine is viewed only as a headache, important context can be lost. Pain becomes the focus, while the broader pattern fades into the background. Recognizing migraine as more than head pain helps explain why symptoms often behave differently from other headaches, and why looking only at pain does not always tell the full story.
How to Think About Migraine vs Headache Going Forward
One useful way to think about migraine and headache is to see them as different experiences. Headache refers to pain felt in the head, whereas migraine refers to a broader neurological state that can include pain but is not defined by it. This distinction helps explain why migraines can look and feel so different from one person to the next, and why pain alone does not always tell the full story.
Severity is often assumed to separate migraine from other headaches, but this assumption can be misleading. Some migraines involve relatively mild head pain yet cause marked sensitivity, fatigue, or cognitive disruption. By contrast, some non-migraine headaches can be intensely painful without involving wider neurological change. For this reason, how disruptive symptoms feel over time often matters more than how sharp or severe a single episode appears.
Migraine patterns tend to be more informative than isolated symptoms. Recurrent features such as sensitivity to light or sound, nausea, fatigue, mental slowing, or a consistent timing pattern often reveal more about whether symptoms reflect migraine than any one attack on its own. Migraine tends to behave as a pattern that unfolds over time, rather than being a series of unrelated pain events.
When migraine is consistently framed as just a headache, the underlying pattern can be missed. This means symptoms may be judged episode by episode, without recognizing the underlying rhythm that connects them. Viewing migraine through a broader lens can help you make sense of varied experiences, lingering symptoms beyond pain, and the limits of simple comparisons with other headaches. This way of thinking helps to explain why head pain is often experienced as a local problem, while migraine is often experienced as part of a broader pattern.
Migraine vs Headache: Key Differences Explained
The table below highlights key differences discussed above, focusing on patterns and overall behavior rather than individual symptoms or severity.
Aspect | Headache | Migraine |
What it describes | Pain felt in the head | A broader neurological state |
Role of pain | Central and defining feature | One possible feature, not always present |
Other symptoms | Usually limited or absent | Often includes sensory sensitivity, fatigue, nausea, or cognitive effects |
Behavior over time | Often isolated or short-lived | Often recurring or patterned over time |
Effect of activity | May improve or remain stable | Often worsens symptoms |
Between episodes | Typically symptom-free | Sensitivity may persist even without pain |
Supporting Migraine Stability with a Structured Nutritional Approach
Migraine sensitivity reflects how the brain manages energy demand, oxidative load, and cumulative stress over time. When these systems are strained, tolerance narrows, making symptoms easier to trigger, slower to settle, or more likely to extend beyond pain alone.
This understanding of migraine has led to interest in nutritional strategies that support the brain’s underlying energy and regulatory needs, rather than focusing only on symptom relief. Brain Ritual® was developed within this framework as a medical food designed specifically for migraine through targeted nutrition.
A central feature of Brain Ritual® is the inclusion of ketone bodies, specifically beta-hydroxybutyrate in a bioavailable mineral salt form, which can be readily used by the brain as an alternative energy source. Ketone metabolism places different demands on energy pathways and is associated with lower production of reactive byproducts, which aligns with the role oxidative stress is thought to play in migraine vulnerability.
Brain Ritual® also includes nutrients commonly discussed in migraine research for their roles in mitochondrial function, antioxidant balance, and nervous system stability, including magnesium, riboflavin, CoQ10, taurine, electrolytes, and trace minerals. These nutrients support processes involved in energy production, oxidative balance, and cellular signaling, all of which are thought to influence migraine sensitivity over time.
Disclaimer: Brain Ritual® is a medical food for the dietary management of migraine and is not intended to diagnose, treat, cure, or prevent any disease. This content is for informational and educational purposes only and is not intended as medical advice.
Frequently Asked Questions
Are headaches and migraines the same?
Headaches and migraines are not the same, even though the terms are often used interchangeably. Headache describes the experience of pain in the head, which can arise through several different mechanisms, such as muscle tension, local inflammation, nerve irritation, or pressure changes in surrounding tissues. Migraine refers to a broader neurological state that can include head pain, but also involves changes in sensory processing, energy regulation, and nervous system responsiveness.
How can you tell if it’s migraine or headache?
The difference between migraine or headache is not always clear from pain alone. Migraine is more likely to involve recurring patterns such as sensitivity to light or sound, nausea, fatigue, mental slowing, or symptoms that follow a familiar timing. Headaches that are not migraine are more often limited to pain itself and tend to resolve without the same wider effects seen in migraine. Looking at how symptoms repeat and evolve over time is usually more informative than judging a single headache episode.
Can you have a migraine without a headache?
Yes. Some people experience migraine activity with little or no head pain. Non-headache symptoms can include visual changes, nausea, dizziness, fatigue, or heightened sensitivity to light or sound. This is one reason migraine is often overlooked or mislabeled, particularly when pain does not match expectations of what a migraine should feel like.
Why are migraines so often mistaken for other headaches?
Migraine is commonly mistaken for tension or sinus headaches because it can cause pressure, facial discomfort, or pain around the eyes. These overlaps occur because migraine affects nerve pathways that also serve the face and sinuses. Migraine symptoms can unfold over time, including early changes known as prodrome, aura in some people, a period when head pain or other symptoms may be present, and lingering effects afterward, often referred to as the postdrome. When attention is focused only on pain location, the broader migraine pattern can be missed, leading to confusion between migraine and other headache types.
Final Thoughts
Migraine and headache are often compared by how severe the pain is, yet many people find that this way of thinking does not fully reflect what they experience. Headache describes pain. Migraine reflects a broader neurological state that shapes how the brain processes sensory input, manages energy, and responds to stress over time. Understanding this difference helps explain why migraine can feel unpredictable, why symptoms may extend beyond pain, and why familiar approaches aimed only at relieving head pain do not always work as expected.
Considering migraine as an ongoing experience can help bring greater clarity. Rather than concentrating on a single episode or symptom, this shifts attention toward how symptoms recur, evolve, and interact across days or weeks. This allows for experiences that do not fit a narrow definition of headache and helps explain why migraine can feel lingering, inconsistent, or difficult to pin down.
Ultimately, recognizing migraine as more than just a headache is about understanding why symptoms behave the way they do, rather than focusing on pain alone.