Table of Contents
- At a Glance
- What Is a Cluster Headache?
- What Is a Migraine?
- How Cluster Headache vs Migraine Symptom Patterns Differ Over Time
- Biological Differences Behind the Pain
- Cluster Headache vs Migraine: Key Differences
- Why Cluster Headache and Migraine Are Often Confused
- Nutritional Strategies for Supporting Brain Energy and Metabolism in Migraine
- Final Thoughts
At a Glance
|
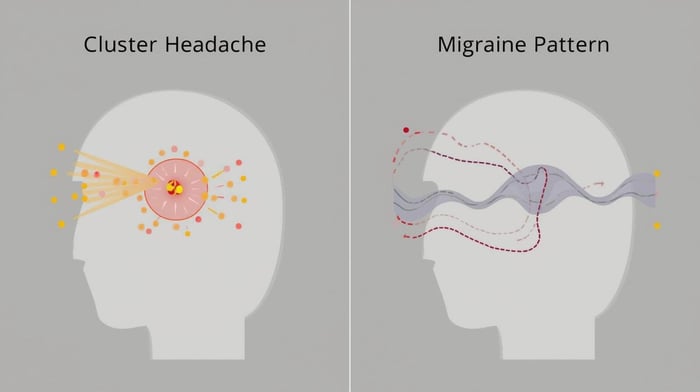
Cluster headache and migraine are distinct neurological conditions. Because both may cause severe head pain centered around the eye or temple, they can be difficult to tell apart. The overlap in pain location and intensity can obscure important differences in how these conditions behave.
Looking beyond intensity alone brings those differences into clearer focus. The contrast between cluster headache vs migraine is less about how painful symptoms feel and more about the timing, progression, and overall structure of symptoms. Both conditions follow a distinct course, shaped by different biological processes and rhythms.
Paying attention to when symptoms appear, how they evolve, and what accompanies the pain makes these differences easier to recognize. This helps explain why cluster headache and migraine may seem similar, yet behave very differently once their broader patterns are considered.
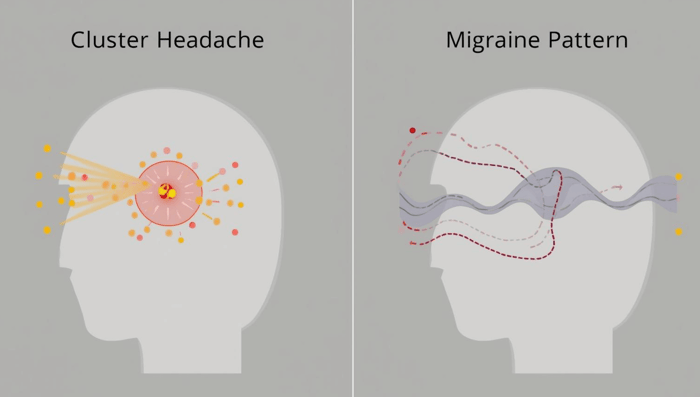
What Is a Cluster Headache?
A cluster headache is a neurological headache disorder characterized by brief, extremely intense attacks of head pain that occur in a distinctive, repetitive pattern. Cluster headaches are much less common than migraines, affecting roughly one in a thousand people (Fischera et al., 2008), and are particularly known for the abrupt onset and intensity of their attacks. Despite their rarity, cluster headaches follow a distinctive pattern that sets them apart from other headache types.
Cluster headache belongs to a group of primary headache disorders known as trigeminal autonomic cephalalgias, a classification defined by severe unilateral pain accompanied by prominent autonomic symptoms. Pain is typically strictly one-sided and most often centered around or behind one eye, or at the temple. Attacks tend to begin suddenly, reach peak intensity quickly, and resolve within a relatively short window, usually lasting between 15 minutes and 3 hours. During a cluster phase, attacks may occur once or multiple times per day, often following a predictable schedule.
A defining feature of cluster headache is the presence of prominent autonomic symptoms (involving nerve systems that control automatic functions) on the affected side of the face. These may include tearing of the eye, nasal congestion or runny nose, eyelid drooping, facial flushing, or a sense of pressure around the eye. These symptoms reflect activation of nerve pathways that run alongside pain signaling networks in the head and face.
Cluster headaches get their name from the way attacks occur in groups, or clusters, over time. During these cluster phases, attacks recur frequently over weeks or months, followed by periods of remission when symptoms are absent. Although the length of both active clusters and remission phases varies between individuals, the clear separation between these phases is a hallmark of the condition.
A further distinguishing difference between cluster headache and migraine lies in behavior during attacks. Unlike migraine, where people often prefer to lie still, cluster headache attacks are commonly associated with marked restlessness. People may often pace, rock, or feel unable to sit or lie down comfortably while pain is present. This behavioral pattern reflects the intensity and sudden onset of symptoms rather than being a specific response to sensory sensitivity.
Taken together, the abrupt onset, short duration, prominent autonomic features, and cyclical pattern of cluster headache help differentiate it from other headache types, such as migraine and tension headaches. These structural features help explain how cluster headache behaves and why it is often experienced as a sharply defined, time-bound condition.
What Is a Migraine?
Migraine involves changes in brain responsiveness that extend beyond head pain. Although pain is a feature shared with cluster headache, migraine is defined by broader differences in how the brain processes sensory input, regulates energy, and responds to internal and external stress.
Migraine pain is often described as throbbing or pulsating and is commonly felt on one side of the head, though it can also be bilateral or shift sides between attacks. In contrast to cluster headache, migraine attacks usually develop more gradually, may fluctuate in intensity, and often last hours to days, with 4 to 72 hours being common. Physical activity, bright light, sound, strong smells, visual motion, or sustained cognitive effort frequently worsen symptoms rather than relieving them.
Migraine is commonly accompanied by neurological symptoms beyond head pain. These may include sensitivity to light or sound, motion sensitivity, nausea, fatigue, dizziness, or cognitive slowing. Some people experience migraine with aura, involving temporary neurological symptoms such as visual disturbances, tingling, or speech changes. Migraine does not require aura, and some people may experience aura without headache or have aura episodes occur more than once in close succession.
Migraine symptoms often unfold as a pattern rather than as a single event. Early prodromal changes such as fatigue, mood shifts, or increased sensory sensitivity may appear before head pain begins, followed by a period of more prominent symptoms, and then a postdrome recovery phase in which sensitivity or tiredness may linger even after pain has eased. This extended progression helps explain why migraine can feel disruptive even when head pain itself is not severe.
Another defining characteristic of migraine is its sensitivity to cumulative strain. Disrupted sleep, missed meals, hormonal changes, sustained mental effort, sensory overload, and stress can all influence how migraine develops and how long symptoms persist. Rather than being triggered by a single factor in isolation, migraine often reflects a brain operating closer to its tolerance threshold, where everyday demands are more likely to provoke symptoms.
This distinction helps separate migraine from other headache types, including cluster headache. Rather than presenting as a sharply defined, time-bound attack, migraine tends to behave as a fluctuating neurological process that develops and resolves over longer periods.
How Cluster Headache vs Migraine Symptom Patterns Differ Over Time
One of the clearest ways to tell cluster headache vs migraine apart is by looking at how symptoms behave over time. Although both involve head pain, their onset, duration, and recovery patterns differ.
Cluster headache follows a highly structured pattern. Attacks typically begin abruptly, reach peak intensity quickly, and resolve within a short window, often within a few hours. During active cluster phases, attacks recur in a predictable rhythm, sometimes at similar times of day or night. Between attacks, symptoms often settle fully until the next cycle begins.
Migraine tends to unfold more gradually and over longer periods. Symptoms may build, fluctuate, and shift in character over hours or days, with head pain not always remaining the dominant feature. Sensory sensitivity, fatigue, nausea, or cognitive slowing may become more prominent at different stages of an attack.
Recovery also differs. Cluster headache attacks often resolve cleanly once the episode ends. Migraine, by contrast, commonly involves lingering effects such as sensitivity or mental fatigue, even after pain has eased, making individual episodes harder to define.
These differences in timing, fluctuation, and recovery help explain why cluster headache is often sharply time-bound, compared with the more prolonged course typical of migraine.
Biological Differences Behind the Pain
Although cluster headache and migraine can both involve severe head pain, different biological processes shape how each condition develops and behaves.
What causes cluster headaches?
Cluster headaches are linked to abnormal activity in brain regions involved in circadian rhythm regulation, particularly the hypothalamus, and disruptions in melatonin secretion have been observed during active cluster periods (Kandel and Mandiga, 2023). This helps explain why attacks often occur in predictable cycles, frequently at similar times of day or night.
This circadian vulnerability also helps explain why certain external factors can provoke attacks during active cluster periods. Alcohol is a well-recognized trigger, often provoking attacks within a short time frame. Strong odors, such as solvents or perfume, and disruptions to sleep timing, are also reported to trigger cluster headache attacks in susceptible individuals. These triggers usually provoke symptoms only during active cluster phases.
Changes in hypothalamic signaling are known to influence pain pathways connected to the trigeminal nerve, the main sensory nerve supplying the face and eye.
This interaction forms the basis of the trigeminal autonomic reflex, a defining mechanism in cluster headache. Activation of this pathway links pain signaling with autonomic responses in the face, producing characteristic symptoms such as tearing, nasal congestion, eyelid drooping, or facial flushing on the affected side. These changes are part of the core attack mechanism rather than secondary effects.
Neurochemical changes, including altered signaling involving histamine, serotonin, and orexin, are also thought to contribute to cluster headaches and may help explain the abrupt onset, short duration, and highly stereotyped nature of episodes.
Migraine biology and energy sensitivity
Migraine involves broader changes in how the brain regulates sensory input, energy demand, and neural excitability. Rather than arising from a single focal trigger, migraine reflects a state in which the brain becomes more responsive to routine internal and external demands.
Growing evidence points to altered brain energy metabolism as a key factor (Del Moro et al., 2022). During migraine, neurons may struggle to meet energy demands efficiently, particularly under sustained cognitive, sensory, or metabolic load. This reduced energy flexibility can lower the threshold for symptom activation and contribute to the fluctuating, multi-phase nature of migraine.
Oxidative stress is also frequently discussed in migraine research. When energy demand exceeds supply, reactive oxygen species may accumulate, placing additional strain on neuronal function (Gross et al., 2021). This metabolic strain lowers tolerance to additional demands, helping explain why migraine is often sensitive to cumulative factors such as poor sleep, missed meals, hormonal shifts, or prolonged mental effort.
Why the experience differs
These biological differences help explain why cluster headache and migraine are experienced so differently. Cluster headache is driven by tightly regulated, highly specific activation of pain and autonomic pathways, resulting in attacks that are intense, unmistakable, and clearly delineated.
Migraine, by contrast, reflects broader shifts in brain regulation that affect sensory processing, energy balance, and stress responsiveness. As a result, symptoms often feel less sharply defined, with changes that emerge gradually, overlap, and linger beyond the point when head pain itself has eased.
Cluster Headache vs Migraine: Key Differences
Although cluster headache and migraine are both neurological conditions, they differ markedly in how attacks begin, how long they last, and how symptoms behave across an attack. Focusing on the structure of attacks, rather than pain intensity alone, often offers the clearest way to distinguish between them.
The table below summarizes the main differences between cluster headache and migraine. These reflect common patterns and help explain why the two conditions can initially feel similar yet behave very differently over time.
Migraine vs Cluster Headache: Key Differences
Feature | Cluster Headache | Migraine |
Underlying nature | A neurological headache disorder characterized by short, intense attacks with prominent autonomic involvement | A broader neurological state involving altered sensory processing, energy regulation, and pain modulation |
Typical attack duration | Short-lasting attacks, usually 15 minutes to 3 hours | Attacks often last hours to days (4 to 72 hours is common) |
Attack timing | Occurs in predictable cycles (clusters), often at the same time of day or night | Timing is more variable and influenced by internal and external factors |
Pain location | Strictly one-sided, usually centered around one eye or temple | Often one-sided, but can shift sides or involve the whole head |
Pain intensity | Extremely severe, sharp, or piercing | Variable, ranging from mild to severe |
Autonomic symptoms | Common and defining, including tearing, nasal congestion, eyelid drooping, or facial flushing | May occur, but are usually less prominent and not defining |
Sensory sensitivity | Typically minimal, and not a defining feature of attacks | Common and often prominent, including sensitivity to light, sound, or movement |
Observed behavior during attacks | Marked restlessness, with difficulty sitting or lying still | Preference for rest, quiet, and reduced stimulation |
Sex distribution | More common in men (male predominance) | More common in women (female predominance) |
Pattern between attacks | Distinct attack-free periods between cluster cycles | Sensitivity or fatigue may persist even without head pain |
These differences help clarify why cluster headache is often experienced as a sharply defined, time-bound condition, while migraine behaves as a more fluctuating neurological pattern that develops and resolves over longer periods.
Why Cluster Headache and Migraine Are Often Confused
Head pain is often discussed in broad terms, with cluster headache, migraine, and tension headache frequently grouped together, even though they arise from different mechanisms and follow distinct symptom patterns. Severe or recurring head pain is often assumed to be migraine, even when the pattern of symptoms points to a different headache type.
Overlapping symptoms can add to this confusion. Both cluster headache and migraine can cause intense one-sided pain, involve facial discomfort, and significantly disrupt daily function.
Autonomic symptoms such as tearing or nasal congestion may appear in both conditions. They are defining in cluster headache, but tend to be more variable in migraine. Neck pain, scalp tenderness, or pressure-like discomfort can further blur distinctions, especially when tension-type or sinus-related headache is also part of the picture.
Symptom variability is also a common source of confusion. Migraine does not always present with classic throbbing pain and can sometimes involve shorter or sharper attacks. Cluster headache, by contrast, is unfamiliar to many people due to its rarity. If timing, attack structure, and associated symptoms are not considered, these conditions can appear more similar than they are, which is why broader comparisons such as migraine vs headache are often helpful for context.
Recognizing underlying patterns helps explain why cluster headache and migraine behave differently, even when head pain is the shared complaint.
Nutritional Strategies for Supporting Brain Energy and Metabolism in Migraine
Migraine involves changes in brain energy regulation, oxidative balance, and sensory sensitivity, which have led to interest in nutritional strategies alongside lifestyle and medical approaches. This reflects growing research linking migraine vulnerability to metabolic strain and reduced energy flexibility in the brain.
Brain Ritual® was developed with this whole-brain view of migraine in mind. Its formulation includes ketone bodies, which provide an alternative energy source for the brain, alongside nutrients commonly discussed in migraine research for their roles in mitochondrial function and oxidative stress balance. These include beta-hydroxybutyrate (BHB), magnesium, riboflavin, and CoQ10, all of which have been widely studied in relation to energy metabolism and antioxidant support.
This approach focuses on factors that may contribute to cumulative migraine sensitivity, rather than the tightly timed autonomic mechanisms that drive conditions such as cluster headache.
For those exploring a structured nutritional option as part of a broader migraine management plan, Brain Ritual® reflects an understanding of migraine as more than isolated head pain, with a focus on underlying neurological and metabolic patterns.
Disclaimer: Brain Ritual® is a medical food for the dietary management of migraine and is not intended to diagnose, treat, cure, or prevent any disease. This content is for informational and educational purposes only and is not intended as medical advice.
Final Thoughts
Although migraine and cluster headache may look similar on the surface, they are fundamentally different experiences. Pain intensity alone rarely tells the full story. Symptom onset, progression, and resolution provide a more reliable way to understand what is happening.
Cluster headache tends to follow a sharply defined course, with attacks that arrive suddenly, repeat in structured cycles, and then recede. Migraine reflects a broader neurological process, where symptoms build, fluctuate, and linger beyond head pain itself. Taken together, these patterns help explain why cluster headache and migraine may appear similar, yet function very differently.